Best Bottles for Breastfed Babies: Top Options and Cost Guide

Feeding decisions can feel stressful, especially when breastfeeding is going well, and a bottle suddenly becomes necessary. Many parents start searching for the best bottles for breastfed babies because they want something that supports nursing rather than interferes with it. The challenge is that many bottles claim to be “breast-like,” but not all actually support how babies feed.
Small details like nipple shape, flow speed, and latch depth can influence how easily a baby moves between breast and bottle. Choosing the best bottles for breastfed babies means looking past marketing and focusing on designs that work with your baby’s natural feeding rhythm.
In this guide, you will learn how to identify supportive bottle features, which options work best for breastfed infants, and how to introduce a bottle without disrupting nursing.
Key Takeaways
- Protect Natural Feeding Patterns: Choose bottles that preserve natural sucking rhythm and help babies recognize when they are full, not ones marketed as “most like breast.”
- Flow Controls Preference: Fast milk flow drives bottle preference. Controlled, slow flow protects breastfeeding mechanics.
- Shape Influences Latch Quality: Gradual slope nipples support a deeper latch and better tongue positioning than short, bulb-shaped designs.
- Introduction Requires Strategy: Timing, positioning, and consistent pumping prevent nursing disruption during bottle transition.
- Verify Pump Insurance Eligibility: Most plans cover breast pumps as DME; confirm eligibility and in-network suppliers to avoid delays.
Why Choosing the Right Bottle Matters for Breastfed Babies
For a breastfed baby, a bottle is not simply a container. It changes how the mouth, airway, and brain coordinate feeding. The wrong design can alter muscle patterns, breathing rhythm, and appetite control. The right bottle protects breastfeeding mechanics while supporting safe, regulated intake.
Bottle choice can affect several natural feeding functions, including mouth muscle use, breathing during feeding, milk flow control, caregiver feeding habits, and how babies recognize fullness.
- Preserving Suction Mechanics: Babies create gentle suction inside their mouths to pull milk from the breast. Some bottle nipples release milk without that effort.
- Suck-Swallow-Breathe Rhythm: Babies naturally suck, swallow, and breathe in a repeating pattern during feeding.
- Preventing Flow Preference: Faster bottle flow reduces feeding effort. Babies may prefer this lower workload, weakening breast suction strength and interfering with effective milk transfer at the breast.
- Reducing Air Swallowing and Reflux: Some babies swallow extra air during feeds. Bottles with uneven milk flow or poor venting can increase gas, stomach pressure, and spit-up.
- Supporting Natural Fullness Signals: Breastfed babies rely on natural signals that tell them when they are full. Fast bottle flow or pressure to finish a bottle can override these cues.
Choosing a bottle that requires your baby to suck for milk and provides a slow, steady flow helps support natural feeding rhythms while reducing choking risk and helping babies recognize when they are full.
What Makes a Bottle Suitable for a Breastfed Baby?

A bottle suitable for a breastfed baby must protect mouth muscle development, feeding coordination, and appetite regulation while allowing smooth transitions between breast and bottle. Suitability depends on how closely the bottle supports natural feeding patterns rather than simply resembling a breast in appearance.
Critical design elements determine whether a bottle supports breastfeeding success and safe intake regulation.
- Ducted Nipple Architecture: Breast-inspired nipple design contains narrow internal channels resembling milk ducts in the breast, meaning milk exits through controlled pathways instead of pooling in a hollow reservoir.
- Suction-Activated Milk Flow: Some nipples release milk only when the baby creates gentle suction with their mouth, rather than allowing milk to drip out automatically.
- Controlled Milk Per Sip: This refers to how much milk a baby swallows at once. Smaller, steady sips help babies swallow safely and reduce choking risk.
- Consistent Milk Flow: Flow rate describes how quickly milk comes out of the nipple. A steady, predictable flow helps babies maintain a comfortable sucking and swallowing rhythm.
- Reduced Visual Volume Cueing: Opaque or weighted bottles limit caregiver reliance on visible milk levels, encouraging responsive feeding based on infant satiety cues rather than bottle completion.
A suitable bottle supports natural feeding mechanics, predictable flow, and caregiver responsiveness without overriding a breastfed infant’s natural regulation patterns.
What Are the Best Bottles for Breastfed Babies?
When identifying the best bottles for breastfed babies, selection should focus on nipple slope geometry, controlled low flow rates, latch depth support, and stable milk transfer. No bottle recreates human breast tissue, but certain designs better preserve breastfeeding mechanics and mouth muscle patterns.
Based on lactation consultant guidance and feeding research, the following bottles align most closely with natural feeding patterns:
Comparative Table: Best Bottles for Breastfed Babies
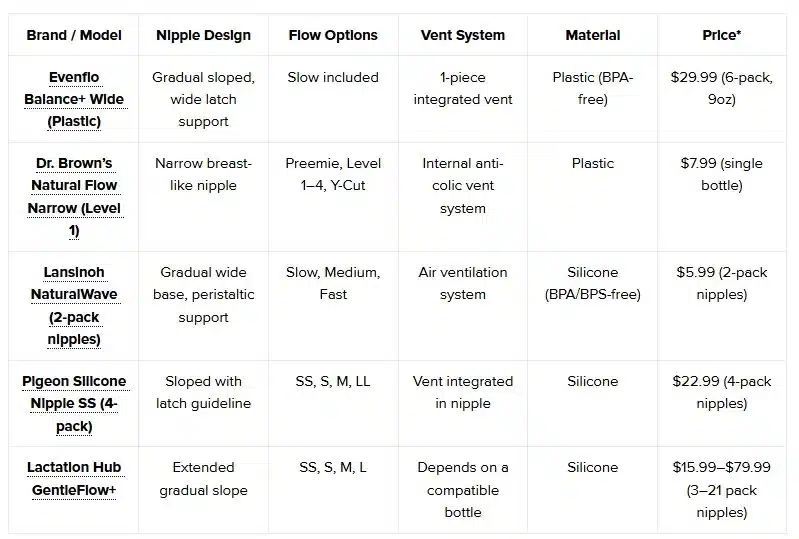
*Prices reflect website listings at the time of writing and may vary by retailer.
-
Evenflo Balance Plus

Evenflo 🍼 Balance + Bottles for Breastfed Babies – Evenflo Feeding
Evenflo Balance Plus is designed with a gradual, breast-like nipple slope to support deep latch formation. It is widely recommended by lactation professionals for babies who alternate between breast and bottle. Both Wide and Standard neck options are available to match infant oral anatomy.
Features:
- Gradual Sloped Nipple: Tapered silicone design encourages wide mouth opening and lip flanging, meaning lips turn outward instead of curling inward.
- Printed Flow Identification: Flow rate (Slow, Medium, Fast) is molded onto the nipple base, reducing confusion when selecting appropriate resistance levels.
- One-Piece Integrated Vent: Built-in vent minimizes air ingestion without complex internal parts, supporting smoother milk transfer and easier cleaning.
Best Use Case: Ideal for breastfed infants needing wide latch support and consistent slow flow while transitioning between direct breastfeeding and occasional bottle feeds.
-
Dr. Brown’s Natural Flow Anti-Colic Options+ (Narrow)

Dr. Brown’s Natural Flow Anti-Colic Options+ Narrow Baby Bottle, 8 oz/ – Dr. Brown’s India
Dr. Brown’s Natural Flow Narrow bottle is widely used in hospitals and NICUs for controlled feeding support. It features a patented internal vent system designed to regulate pressure inside the bottle.
The Narrow version is often preferred for smaller oral anatomy and preterm infants.
Features:
- Internal Vent System: Two-piece vent prevents vacuum buildup inside the bottle, stabilizing milk flow and reducing air ingestion linked to colic and reflux.
- Level-Based Flow Control: Preemie and Level 1 nipples provide measurable slow-flow rates, reducing the risk of flow overload and swallow incoordination.
- Narrow Nipple Profile: Slimmer base supports controlled latch depth in infants with smaller oral cavities or immature mouth muscle tone.
Best Use Case: Well-suited for breastfed newborns, preterm infants, or babies with reflux who require consistent slow flow and pressure-regulated milk delivery.
-
Lansinoh NaturalWave®

Lansinoh NaturalWave Bottle Nipples – 2 Count
Lansinoh NaturalWave® is designed to support babies transitioning between breast and bottle. The nipple shape encourages similar tongue and jaw movement patterns used during breastfeeding. It is frequently recommended for families aiming to protect latch consistency.
Features:
- Peristaltic Tongue Support: Designed to encourage peristalsis, meaning wave-like tongue motion that compresses and elevates the nipple during breastfeeding.
- Gradual Wide Base: Sloped base promotes wide gape and lip flange, reducing shallow latch patterns often seen with short, bulb-shaped nipples.
- Air Ventilation System: Integrated vent reduces negative pressure buildup and limits excess air intake associated with gas and spit-up.
Best Use Case: Appropriate for breastfed infants transitioning between breast and bottle who need latch consistency and moderate flow control without abrupt milk release.
-
Pigeon Silicone Nipple (SS)

Buy Softlatch Peristaltic plus Nipple Case SS Online | Pigeon India
Pigeon Silicone Nipple (SS) is designed for newborns requiring ultra-slow, controlled milk transfer. Its structured slope supports deep latch positioning and oral stability. The SS designation stands for “Super Slow,” indicating minimal flow resistance for early feeding stages.
Features:
- Latch Line Guide: Printed alignment mark indicates optimal nipple depth, helping caregivers position the nipple to support proper lip flange and tongue placement.
- Ultra-Slow Milk Flow: SS flow releases milk very slowly, helping babies swallow comfortably and preventing too much milk from entering the mouth at once.
- Soft-Touch Silicone Structure: Medical-grade silicone allows controlled collapse under suction while maintaining structural integrity to avoid flattening during active sucking.
Best Use Case: Ideal for newborn or breastfed infants needing very slow, controlled flow with structured latch guidance to support coordinated sucking and swallowing.
-
Lactation Hub GentleFlow+

GentleFlow+ Bottle Nipple with Gradual Slope for Breastfed and Combo Fed Babies
GentleFlow+ is a lactation consultant–designed nipple created specifically for breastfed and combo-fed infants. Its defining feature is a gradual slope that encourages deeper latch mechanics. Multiple progressive flow levels allow developmentally appropriate milk resistance.
Features:
- Gradual Tapered Slope: Extended base-to-tip incline promotes tongue cupping, meaning the tongue forms a supportive bowl shape during sucking.
- Super Slow Flow Option (SS): Designed for 0–3 months, offering reduced flow velocity to protect feeding rhythm and prevent flow preference.
- Multi-Stage Flow Progression: SS, S, M, and L options provide age-based resistance changes without abrupt increases in milk transfer speed.
Best Use Case: Appropriate for breastfed or combo-fed infants needing structured latch support and very slow, developmentally matched flow control during breast-to-bottle transitions.
Each of these bottles prioritizes controlled flow, deep latch support, and natural feeding patterns rather than marketing claims of being “most like breast.”
Is Nipple Confusion Real or Is It Flow Preference?
Hearing that a baby may become “confused” after one bottle can feel overwhelming. The reassuring truth is that most feeding challenges after bottle introduction are not neurologic confusion. In clinical practice and lactation research, the issue is usually behavioral learning linked to milk delivery speed, not loss of breastfeeding ability.
To clearly distinguish the two concepts, examine the mechanisms involved.
- True Muscle Coordination Disruption: Real nipple confusion would mean the baby struggles to coordinate tongue, jaw, and mouth movements needed for feeding. This is rare in healthy full-term babies.
- Behavioral Conditioning Response: Babies learn through repetition. Faster milk flow creates positive reinforcement, meaning the brain associates bottles with quicker reward.
- Effort-Reward Ratio: Breastfeeding requires sustained sucking before the milk ejection reflex begins. Bottles with immediate flow reduce required effort, altering feeding expectations.
- Swallow Timing Adaptation: Infants adapt swallow frequency to flow rate. Faster flow increases swallow frequency and decreases pause intervals, changing feeding rhythm patterns.
- Feeding State Association: Babies may associate bottles with satiety achieved more quickly. This can influence preference without affecting breastfeeding skill or latch capability.
Current evidence suggests most breast refusal after bottle use reflects learned preference for faster reward, not inability to breastfeed.
How to Introduce a Bottle to a Breastfed Baby Without Disrupting Nursing

Introducing a bottle can feel delicate, especially when nursing is going well. The goal is not simply bottle acceptance. The goal is to preserve latch quality, milk supply, and coordinated sucking patterns while adding flexibility. When timing, equipment, and technique align, most babies transition smoothly without affecting breastfeeding.
Successful introduction depends on structured steps that protect natural feeding patterns.
- Time It After Supply Stabilizes: Introduce between 2–4 weeks postpartum once milk supply regulates. Supply regulation means hormone-driven production shifts to demand-driven production.
- Use Low-Volume Practice Feeds: Start with a small amount during calm, alert states rather than peak hunger. This prevents stress-driven sucking and frantic latch behaviors.
- Match Feed to Pump Session: Pump during or within 30 minutes of bottle feeding. This protects prolactin signaling, the hormone that supports ongoing milk production.
- Control Feeding Positioning: Hold baby upright at 60–90 degrees. This supports suck-swallow-breathe coordination and reduces the risk of milk going toward the airway or causing coughing.
- Limit Session Duration: Keep feeds moderate in length. Very fast feeds increase flow conditioning, while overly prolonged feeds can lead to oral fatigue and inefficient sucking patterns.
Consistency matters. Offer a bottle several times weekly once accepted to preserve skill memory without replacing breastfeeding sessions unnecessarily.
What to Do If a Breastfed Baby Refuses the Bottle
Bottle refusal can feel discouraging, especially when a return to work or medical need is approaching. In most healthy babies, refusal is not stubbornness. It reflects sensory preference, caregiver association, or unfamiliar oral mechanics. With calm repetition and strategic adjustments, acceptance usually improves.
When a breastfed baby refuses a bottle, focus on targeted behavioral and sensory shifts.
- Change The Feeding Caregiver: Babies strongly associate the breastfeeding parent with nursing. Having another caregiver offer the bottle reduces the expectation of direct breastfeeding.
- Adjust Behavioral State: Offer during quiet alert periods. Quiet alert means eyes open, relaxed limbs, not crying or deeply sleepy.
- Modify Sensory Input: Warm the nipple under water before feeding. Silicone temperature influences tactile acceptance and initial suck reflex activation.
- Encourage Self-Initiated Latch: Stimulate the upper lip to trigger the rooting reflex. Rooting is the automatic head-turning and mouth-opening response in infants.
- Desensitize Outside Feeding: Allow non-feeding exploration of the nipple. Repeated oral exposure reduces novelty-related rejection.
If refusal persists, consider flow resistance or nipple firmness mismatch. Some infants require firmer silicone to generate adequate sensory feedback for coordinated sucking.
In older infants, open cup or straw cup introduction may be appropriate if developmentally ready.
How Many Bottles Are Needed for a Breastfed Baby?

It is completely normal to wonder how many bottles are actually necessary. The answer depends on separation time, pumping frequency, and washing capacity. Breastfed babies typically take smaller volumes per feed than formula-fed infants, so oversized bottle sets are rarely needed.
Bottle quantity should match feeding logistics, not marketing bundles.
- Start with Single Trials: Purchase one bottle from a few brands first. This prevents bulk investment before confirming nipple shape and flow compatibility.
- Match Bottles To Separation Hours: Plan one bottle per missed nursing session. Missed session means any feed occurring while the parent and baby are apart.
- Account for Pumping Output: Pumped milk volume per session determines bottle size. Most breastfed infants take moderate volumes rather than progressively larger feeds.
- Consider Cleaning Capacity: Bottles with multi-part vent systems require longer washing time. Extra sets reduce stress during high-demand days.
- Evaluate Storage Workflow: Families storing milk in the refrigerator may prefer additional bottles for rotation between feeding, chilling, and washing cycles.
For occasional bottle use, a small rotation is usually sufficient. For workday separation, the bottle count should mirror the feeding frequency during those hours.
Insurance Covered Breast Pumps: What Parents Need to Know
If pumping is part of your feeding plan, insurance coverage can significantly reduce out-of-pocket costs. Under federal guidelines, most health plans are required to cover a breast pump. The key is understanding eligibility, documentation requirements, and plan-specific limitations before ordering.
Coverage details depend on plan type, timing, and medical necessity criteria.
- Understand Eligibility Requirements: Eligibility determines if your insurance plan covers a pump. Most ACA-compliant plans must provide one pump per pregnancy.
- Prescription or Medical Order: Some insurers require a prescription from an OB-GYN or pediatric provider before approving coverage or shipping equipment.
- In-Network Durable Medical Equipment (DME): Breast pumps are classified as DME. Ordering through an in-network DME supplier reduces claim denials and billing issues.
- Plan-Specific Pump Models: Insurance may cover specific models only. Upgrades to wearable or hospital-grade pumps may require additional payment.
- Timing of Coverage Release: Many plans release pumps at a specific gestational week or postpartum. Ordering too early can delay approval.
Confirming eligibility early in pregnancy prevents last-minute stress. Documentation accuracy and supplier coordination facilitate the approval process.
Final Thoughts
Feeding choices rarely look the same from one family to another, and that flexibility is not a setback. It is part of modern parenting. When bottles are introduced thoughtfully, they can support growth, bonding, and shared caregiving without undermining nursing. Confidence comes from clarity, not perfection. A well-informed plan allows feeding to feel steady rather than stressful.
If pumping is part of your routine, check your Insurance cover early so the equipment is ready when you need it. The right support makes a measurable difference in daily feeding logistics. Guidance, access, and coverage should work together, not create friction.
If you have questions about pumps or coverage options, reach out to us today for personalized assistance.
FAQs
-
Does the “Best Bottle That Mimics Breast” Actually Replicate Breastfeeding Mechanics?
No bottle can fully replicate breastfeeding. The breast releases milk through suction-triggered let-down, while most bottles allow gravity-assisted flow. Look for slow flow and gradual slope support.
-
Are Lactation Consultant-Recommended Bottles Always Wide-Based?
Not necessarily. Many IBCLCs prefer gradual slope nipples over ultra-wide bulb shapes because they support deeper latch and tongue cupping mechanics.
-
What Is the Best Bottle for Exclusively Pumping Parents?
Exclusively pumping families benefit from bottles compatible with pump flanges. Direct pump-to-bottle systems reduce milk transfer steps and preserve volume accuracy.
-
What Is the Best Bottle for a Breastfed Baby Who Refuses the Bottle?
Focus on flow resistance and sensory familiarity. Babies who refuse often respond better to firmer silicone and controlled flow rather than softer, high-drip nipples.
-
Should Breastfed Babies Use Preemie Flow Nipples Even After the Newborn Stage?
Often yes. Preemie or ultra-slow flow maintains active sucking effort and prevents quick milk conditioning, especially for babies alternating between breast and bottle.










