Breastfeeding vs Pumping: Which Feeding Method Works Best?

It is 2 a.m., your baby is crying, and you are trying to figure out the next feeding. Should you nurse right away, or warm the bottle of milk you pumped earlier? Moments like this are when many new moms start thinking seriously about breastfeeding vs pumping.
If you feel unsure which method is easier or better for your baby, you are not alone. Many mothers explore both options while learning what works best for their routine, recovery, and support system. Understanding the real differences between breastfeeding and pumping can make feeding decisions much less stressful.
In this guide, you will learn how the two methods compare, the benefits and challenges of each, and how many families combine both to make feeding more manageable.
Key Takeaways
- In breastfeeding vs pumping, nursing relies on a baby’s suck-swallow-breathe pattern, while pumping uses mechanical suction to express milk for bottle feeding later.
- Even when milk is refrigerated or frozen, it retains important antibodies and nutrients that support infant immunity and healthy development.
- Breastfeeding may involve latch learning and breast discomfort, while pumping requires managing equipment, pumping schedules, and proper milk storage.
- Daily convenience often depends on lifestyle factors such as work schedules, nighttime feeds, and whether caregivers help with feeding.
- Many U.S. insurance plans cover one breast pump per pregnancy, making it easier to maintain pumping routines without additional equipment costs.
Breastfeeding vs Pumping: What Is the Difference
Many new mothers compare breastfeeding and pumping when deciding how their baby will receive breast milk each day. The two methods differ in feeding mechanics, milk expression, and caregiving flexibility, which can influence feeding routines, milk supply management, and how easily other caregivers participate in feeding.
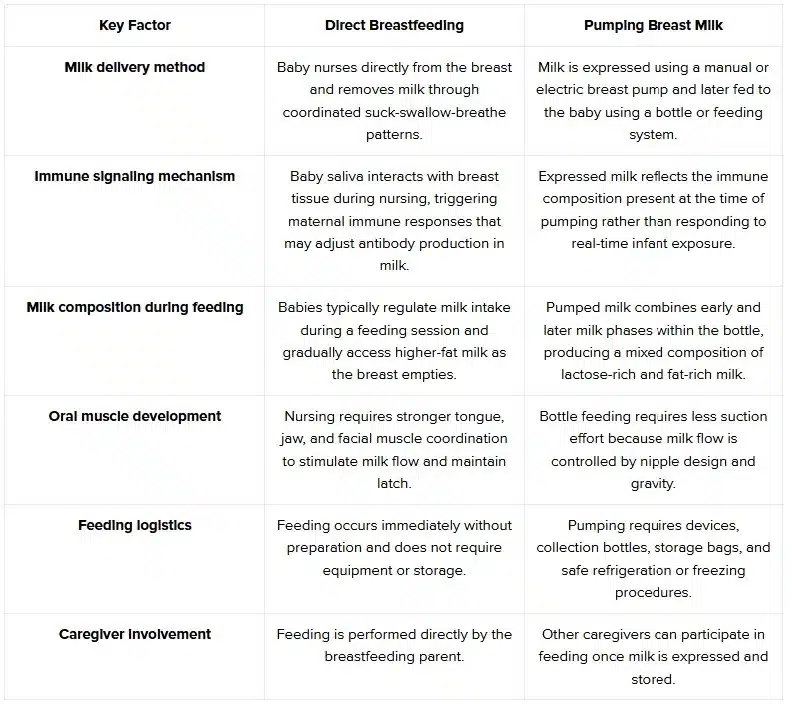
Both methods deliver breast milk, but the feeding experience changes depending on how the milk is expressed and given. Many families choose the approach that best fits their baby’s feeding behavior and their everyday schedule.
If you are starting your breastfeeding journey, learning safe cleaning and storage habits can make feeding routines easier. Read our guide on Breastfeeding Hygiene Tips For New Mothers.
Is Pumped Breast Milk as Healthy as Nursing

Many mothers worry that pumping might reduce the health benefits of breast milk compared with direct nursing. Pumped milk still delivers powerful nutrition and immune protection. The main differences relate to how milk is stored, handled, and exposed to air, which can influence living immune cells and certain protective compounds.
Several biological factors explain how expressed breast milk compares with milk consumed directly during breastfeeding.
- Living Immune Cells: Fresh breast milk contains living immune cells called leukocytes, which help destroy bacteria and viruses. Freezing or pasteurizing milk reduces the number of these active protective cells.
- Beneficial Bacteria for Gut Health: Breast milk naturally contains helpful bacteria that support a baby’s developing gut microbiome, which means the community of microbes that supports digestion and immunity.
- Vitamin Stability During Storage: Some vitamins, including vitamin C and certain antioxidants, gradually decline during refrigeration or freezing, although proteins, fats, and lactose usually remain stable.
- Antibodies That Fight Infection: Breast milk contains antibodies such as secretory immunoglobulin A (IgA), proteins that protect babies from respiratory and digestive infections even after milk is refrigerated.
- Handling and Temperature Effects: Reheating milk multiple times or leaving it at room temperature too long can reduce sensitive bioactive compounds that support immune protection and early digestive development.
Pumped milk still provides excellent nutrition and immune protection for babies. Even though fresh milk contains some additional living components, expressed breast milk remains one of the healthiest feeding options.
Many moms experience soreness or discomfort during the early weeks of feeding. Understanding what is normal and when to seek help can bring real relief. Learn more in Common Breastfeeding Pain Questions and Solutions.
Common Challenges New Mothers Face with Breastfeeding vs Pumping
The early weeks of feeding can feel overwhelming for many mothers, especially while learning the differences between breastfeeding and pumping. Each method comes with specific physical, scheduling, and equipment-related challenges. Understanding these hurdles helps parents prepare practical solutions and seek support when feeding routines feel difficult.
The table below outlines practical challenges mothers commonly experience with each feeding method.
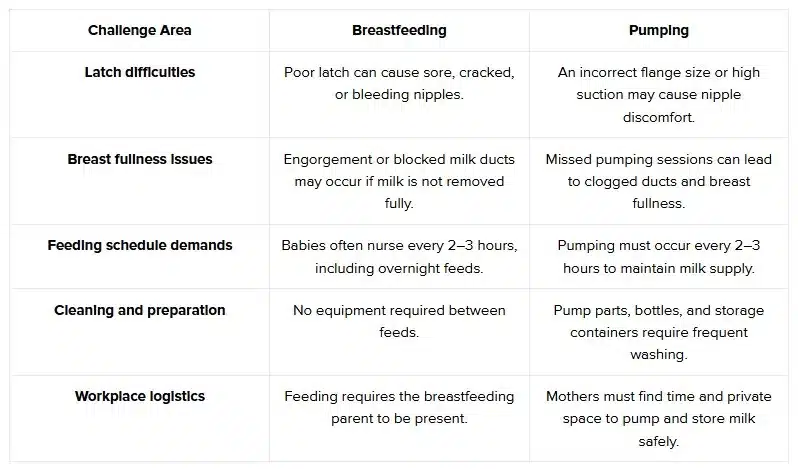
Both breastfeeding and pumping involve an adjustment period. With time, practice, and the right support, most mothers develop a feeding routine that feels manageable for their baby and family.
Which Feeding Method Is More Convenient

Convenience often shapes how mothers choose between breastfeeding and pumping during the first months after birth. Each method fits daily routines differently depending on work schedules, nighttime feeding patterns, and caregiving support. Understanding these practical differences helps parents decide which option feels manageable for everyday life.
Several day-to-day factors influence how convenient breastfeeding or pumping may feel during newborn care.
- Immediate Milk Access: Breastfeeding provides milk instantly at body temperature without preparation, warming bottles, or measuring portions, which simplifies quick feeds during nighttime wake-ups or travel.
- Shared Feeding Support: Pumping allows stored milk to be fed by partners or caregivers, giving mothers time to sleep, recover postpartum, or attend work or appointments.
- Feeding Schedule Control: Pumping allows parents to plan milk expression sessions around work shifts or childcare schedules, while breastfeeding usually follows a baby’s hunger cues.
- Travel and Mobility: Breastfeeding requires no equipment, making short outings easier, while pumping often involves carrying pumps, storage containers, and cooling packs for milk safety.
- Milk Supply Flexibility: Pumping can build a stored milk supply for emergencies or separations, while breastfeeding depends on the mother being physically present for each feeding.
Convenience varies for every family. Many mothers find that combining breastfeeding and pumping offers both flexibility and immediate feeding support.
If you are considering pumping regularly, choosing the right pump can make a big difference in comfort and convenience. Explore the differences in Wearable Breast Pump vs Regular Pumps Pros, Cons, and Differences.
Can You Combine Breastfeeding and Pumping
Many mothers choose to combine breastfeeding and pumping to balance bonding with flexibility. This approach allows babies to nurse directly while also receiving expressed milk when caregivers help with feedings or when mothers return to work. With the right routine, both methods can support a healthy milk supply.
Several feeding strategies help mothers successfully combine nursing and pumping during the first months after birth.
- Pump When Baby Would Normally Nurse: Pumping sessions scheduled at the same time a baby would typically feed help maintain the supply-and-demand signals that regulate breast milk production.
- Nurse and Pump in the Same Session: Some mothers nurse on one breast while pumping the other, which stimulates milk release and can increase the total amount expressed.
- Use Paced Bottle Feeding: Holding the bottle horizontally and using slow-flow nipples helps babies alternate between breast and bottle without developing a preference for faster bottle flow.
- Build a Stored Milk Supply: Pumping extra sessions during the day allows mothers to create a small freezer supply of milk for workdays, appointments, or emergencies.
Many families find that combining breastfeeding and pumping provides both feeding flexibility and continued access to the biological benefits of breast milk.
How the Right Breast Pump Makes Pumping Easier
Choosing the right breast pump can significantly improve comfort, milk output, and daily pumping routines. Pump design affects suction rhythm, breast fit, and pumping efficiency. When equipment matches a mother’s anatomy and schedule, pumping sessions often become faster, more comfortable, and easier to maintain consistently.
Several technical features determine how effectively a breast pump supports milk expression and long-term pumping comfort.
- Correct Flange Fit: The flange, also called a breast shield, should allow the nipple to move freely in the tunnel. Incorrect sizing can cause friction, nipple swelling, and reduced milk removal.
- Adjustable Suction Levels: Quality pumps allow mothers to control suction strength and rhythm, helping mimic a baby’s natural suck pattern and improving comfort during longer pumping sessions.
- Double Pumping Capability: Electric double pumps express milk from both breasts simultaneously, reducing session time and stimulating higher prolactin hormone release that supports stronger milk production.
- Lifestyle-Compatible Pump Design: Wearable or portable electric pumps allow pumping during work, commuting, or household tasks, making regular sessions easier to maintain without interrupting daily responsibilities.
- Hands-Free Pumping Support: Hands-free pumping bras or wearable collection cups stabilize the pump in place, allowing mothers to relax, hydrate, or care for their baby during milk expression.
A well-fitted pump designed for your routine can make pumping more comfortable and sustainable. The right equipment helps protect milk supply while fitting smoothly into everyday life.
How to Get an Insurance-Covered Breast Pump

Many mothers in the United States can receive a breast pump through health insurance because the Affordable Care Act requires most plans to cover breastfeeding equipment and support. Understanding the process helps parents request coverage early, confirm their eligibility, and avoid delays once the baby arrives.
The following steps outline how mothers typically obtain a breast pump through their insurance plan.
- Verify Insurance Coverage: Most private insurance plans cover one breast pump per pregnancy under the Affordable Care Act preventive care benefit, though pump type and coverage details vary by insurer.
- Confirm Eligibility Timeline: Insurance providers often specify when a breast pump can be ordered. Some plans allow requests during pregnancy, while others approve coverage after the baby is born.
- Choose an Approved Pump Model: Insurance plans usually cover specific pump categories such as manual pumps, standard electric pumps, or hospital-grade pumps, depending on policy terms and medical necessity.
- Submit Insurance Information: Mothers typically provide their insurance details, expected due date, and healthcare provider information through an approved medical supplier who processes the claim.
- Receive Your Pump Shipment: After the claim is approved, the supplier ships the breast pump directly to the mother’s home, often before delivery or soon after the baby arrives.
Ordering through an approved supplier often simplifies the process because the provider verifies coverage and manages insurance paperwork for you.
Final Thoughts
Feeding your baby is rarely a one-size-fits-all experience. As you think through breastfeeding vs pumping, remember that many mothers adjust their approach along the way. What works during the newborn weeks may look different once routines, sleep patterns, and daily schedules begin to settle.
The most important thing is that your baby is nourished and that you feel supported in the process.
If you are still deciding between breastfeeding vs pumping, give yourself permission to learn as you go. With time, guidance from a lactation consultant, and the right tools, many parents discover a feeding rhythm that feels comfortable, realistic, and right for their family.
FAQs
1. Is exclusively pumping vs breastfeeding harder for mothers?
Exclusively pumping vs breastfeeding can feel more demanding because it involves pumping sessions, milk storage, and cleaning equipment alongside bottle feeding.
2. Can nursing vs pumping affect how quickly milk lets down?
Yes. During nursing vs pumping, babies often trigger faster milk let-down through natural suckling patterns, while pumps rely on suction settings.
3. Does pumping vs breastfeeding change how babies accept bottles later?
During pumping vs breastfeeding, babies exposed to bottles early may transition between feeding methods more easily than babies who only nurse.
4. Are there benefits of breastfeeding vs pumping during nighttime feeds?
Benefits of breastfeeding vs pumping at night include faster feeding because milk is available immediately without warming bottles or assembling pumping equipment.
5. Does breastfeeding vs exclusively pumping affect feeding flexibility?
Breastfeeding vs exclusively pumping affects flexibility because pumping allows caregivers to feed the baby, while breastfeeding usually requires the mother’s presence.










