Postpartum Swelling Explained: Why It Happens and How to Reduce It

Some days after birth, the body can feel unfamiliar. Shoes feel tight, fingers feel puffy, and ankles look swollen by evening. Postpartum swelling often shows up right when energy is already low, and emotions are close to the surface. Seeing that extra puffiness can be unsettling, especially when rest feels scarce and recovery feels slow.
It helps to know that postpartum swelling is common while the body shifts fluids, hormones, and circulation back toward its usual balance. Gentle, practical steps can ease discomfort and help you feel more like yourself again. Knowing the difference between normal swelling and warning signs also brings peace of mind during this tender stage.
In this guide, clear answers and simple relief tips are shared to support healing while caring for a newborn.
Key Takeaways
- Postpartum swelling, including postpartum foot swelling and pedal edema, is common as the body shifts extra pregnancy fluid back into circulation.
- Swollen legs and feet after a C-section or edema after a C-section may persist up to three weeks due to surgical IV fluids and reduced early mobility.
- Swelling in feet and ankles differs from breast engorgement. Postpartum edema affects body tissues, while breast swelling relates to milk production and needs different relief.
- Hydration, lower sodium intake, gentle movement, leg elevation, and compression socks help the body gradually reduce fluid retention and ease discomfort.
- One-sided leg swelling, chest pain, severe headache with swelling, or redness with fever are urgent signs that need immediate medical evaluation.
Is Postpartum Swelling Normal After Birth?

Yes, postpartum swelling is a common physiologic response as your body shifts from pregnancy’s circulation patterns back to its pre-pregnancy state. What feels alarming is often your vascular and lymphatic systems recalibrating after months of higher fluid volume.
Types Of Postpartum Swelling
Understanding the type, the signs, and the cause can help make sense of what you are seeing.
1. Feet and Ankle Swelling
Signs: Tight shoes, sock lines that linger, ankles appearing fuller by the end of the day, mild heaviness when walking.
What Is Happening: Extra pregnancy fluid moves downward due to gravity, while circulation and vein tone slowly return to normal after birth.
2. Leg and Lower Body Edema
Signs: Legs feel tight, heavy, or slightly tender, especially after a C-section or long labor; swelling may extend up toward calves or knees.
What Is Happening: IV fluids given during surgery or labor expand tissue fluid levels, and reduced early mobility slows how quickly veins and lymph vessels clear excess fluid.
3. General Postpartum Edema
Signs: Puffy fingers, facial fullness, rings feeling snug, or mild eyelid swelling upon waking.
What Is Happening: Hormonal changes and increased blood volume from pregnancy take time to normalize, leading to temporary fluid retention throughout the body.
4. Pedal Edema Postpartum
Signs: Swelling focused mostly in the feet, worse after standing or sitting for long periods, often improving overnight when legs are elevated.
What Is Happening: Slower lymphatic drainage and decreased muscle movement allow fluid to collect in the lowest parts of the body.
5. Hormone-Related Fluid Retention
Signs: Sudden puffiness in the hands, feet, or face after labor medications like Pitocin, sometimes spreading beyond the local area.
What Is Happening: Hormonal shifts influence blood vessel dilation and fluid balance, causing temporary water retention until levels stabilize.
Each type of swelling has a different pattern, but all reflect the body gradually returning to balance after pregnancy and birth.
How to Reduce Postpartum Swelling at Home

Your body is already working to clear extra pregnancy fluid through urine and sweat. These home strategies gently support circulation, kidney function, and tissue recovery to ease discomfort safely.
-
Stay Well Hydrated
Drinking enough fluids helps your kidneys release retained sodium and excess extracellular fluid. Steady hydration signals your body that it does not need to conserve water.
- Sip water consistently throughout the day rather than drinking large amounts at once, which helps maintain stable blood concentration and supports gradual kidney fluid filtration.
- Monitor urine color as a guide; pale yellow usually reflects adequate hydration supporting fluid balance, while darker urine suggests your body may still be conserving water.
-
Reduce Sodium Intake
Excess sodium pulls water into tissues, increasing puffiness. Lowering hidden salt sources helps your body release stored fluid more efficiently during postpartum recovery.
- Check nutrition labels on packaged foods, since breads, sauces, and frozen meals often contain high sodium levels that quietly contribute to fluid retention.
- Flavor meals with herbs, garlic, lemon, or vinegar instead of salt to reduce sodium load without sacrificing taste during recovery.
-
Increase Potassium-Rich Foods
Potassium helps counterbalance sodium’s fluid-retaining effects. Eating potassium-rich foods supports cellular fluid regulation and reduces excess water staying in surrounding tissues.
- Add foods like baked potatoes, lentils, yogurt, and leafy greens to meals to help your body shift sodium out of cells and reduce swelling.
- Pair potassium sources with balanced meals to support steady absorption rather than relying on supplements without medical guidance.
-
Limit Caffeine Intake

Caffeine can increase urine output initially but may contribute to dehydration later, which signals your body to conserve water and can prolong swelling.
- Swap one caffeinated drink per day with water or herbal tea to reduce dehydration risk without abrupt withdrawal symptoms.
- Drink extra water if you consume caffeine while breastfeeding, since fluid needs are already higher during milk production.
-
Elevate Your Legs
Raising your legs above heart level reduces pressure in lower limb blood vessels, encouraging fluid in swollen tissues to move back into circulation.
- Use pillows to lift calves while lying down so gravity assists venous return rather than allowing fluid to settle in ankles and feet.
- Elevate legs for 15–20 minutes several times daily instead of one long session to support repeated fluid redistribution.
-
Add Gentle Movement
Light activity stimulates muscle contractions that help move both blood and lymph fluid, preventing them from collecting in one area for long periods.
- Take slow, short walks indoors to activate calf and thigh muscles that naturally help pump fluid back toward the heart.
- Perform gentle ankle circles or foot flexing while seated to keep lower-leg circulation active during rest periods.
-
Wear Compression Garments
Compression supports vein walls and reduces fluid leakage into surrounding tissues, especially helpful for persistent ankle and lower leg swelling postpartum.
- Choose graduated compression socks that are snug at the ankle and gradually looser upward to promote upward blood flow.
- Put compression garments on in the morning before swelling worsens, when leg size is closest to baseline.
-
Try Gentle Massage
Light massage encourages lymphatic flow and circulation, helping your body move protein-rich fluid out of swollen areas more efficiently.
- Use soft, upward strokes toward the groin when massaging legs, following natural lymph drainage pathways rather than pressing deeply.
- Apply a light moisturizer before a massage to reduce skin friction and avoid irritation that can increase localized inflammation.
-
Use a Foam Roller Carefully
Foam rolling can stimulate circulation in large muscle groups, which may support venous return and reduce the feeling of heaviness in swollen legs.
- Roll slowly over calf and thigh muscles using gentle pressure to encourage blood flow without causing tissue soreness.
- Avoid rolling directly over joints or areas with visible varicose veins to prevent vessel irritation.
-
Choose Loose, Non-Restrictive Clothing
Tight garments can compress blood vessels and trap fluid in certain areas. Looser clothing supports more natural circulation and fluid movement.
- Avoid tight waistbands or socks that leave deep marks, which indicate restricted blood and lymph flow in that area.
- Opt for breathable fabrics that reduce skin irritation, since inflamed tissues may hold more fluid temporarily.
Your body clears fluid gradually, not overnight. Gentle daily habits that support circulation, hydration, and balanced nutrition can make swelling feel more manageable while recovery continues.
Curious how feeding supports both you and your baby? Learn more in Health Benefits of Breast Feeding
How Long Does Postpartum Swelling Last?
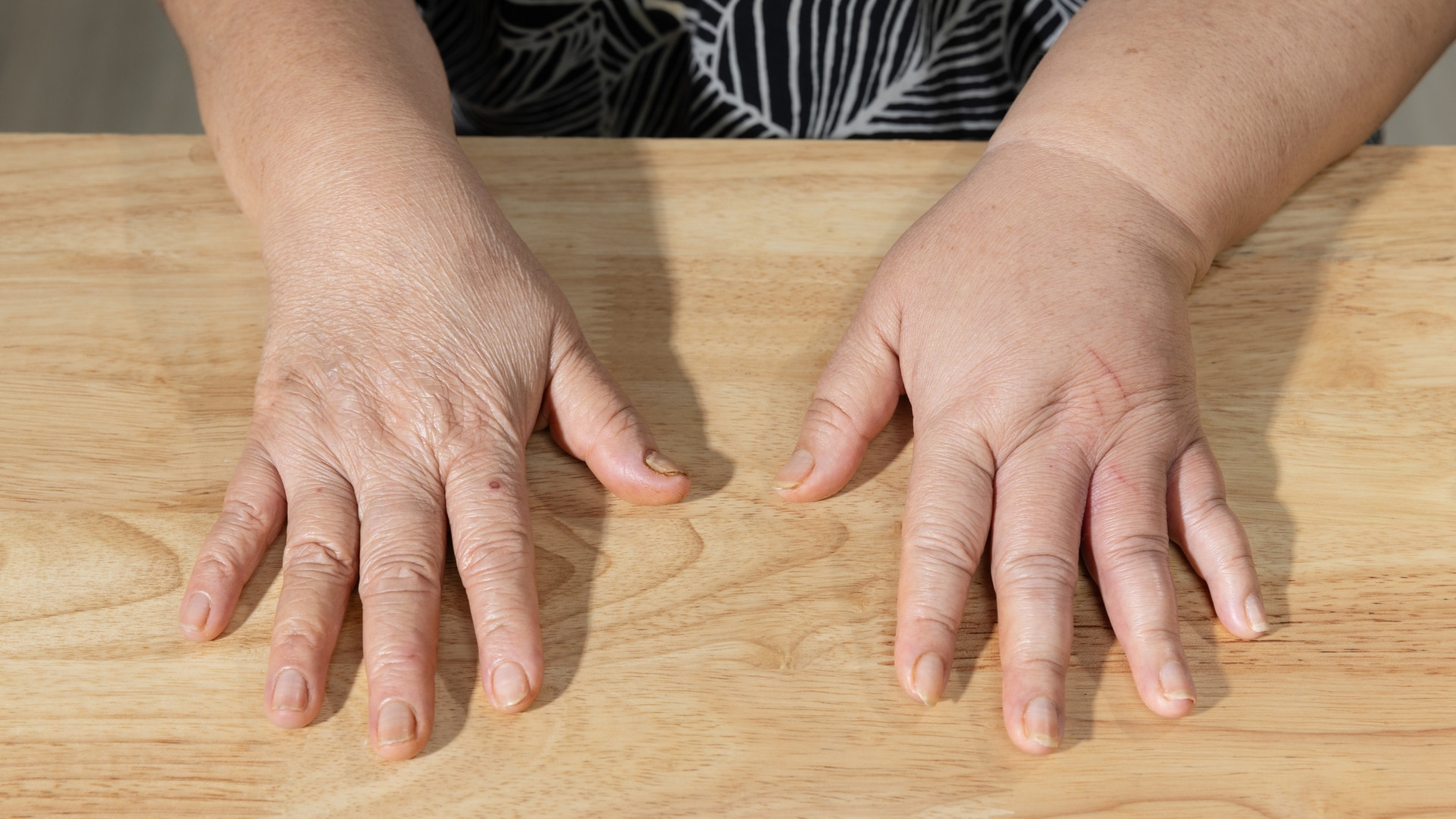
Postpartum swelling does not disappear all at once. It follows your body’s recovery phases as circulation, kidney function, and tissue pressure gradually return to baseline after delivery.
Here is how swelling changes across the postpartum timeline typically:
- Immediate Hours After Birth: Extra pregnancy fluid remains in circulation right after delivery. Mild swelling is common, and providers monitor it closely during this early recovery window.
- First Week Postpartum: Swelling from retained pregnancy fluids typically improves during the first week as your body clears fluid through urine and sweat.
- Subacute Recovery Phase (First 2–6 Weeks): Hormones, circulation, and tissues continue adjusting. Some mild puffiness, especially in feet and ankles, can linger but should steadily decrease.
- After Cesarean Birth: Swelling may last a bit longer due to surgical fluids and reduced mobility in the early days, but gradual improvement is still expected.
- Delayed Recovery Phase (After 6 Weeks): By this stage, fluid-related swelling should be resolved. Ongoing swelling beyond this point should be discussed with a healthcare provider.
Most moms see clear improvement within two weeks, even if mild puffiness lingers a bit longer. Steady reduction matters more than overnight change; your body is unwinding months of fluid buildup.
For a step-by-step look at what recovery can involve, explore Recovering From Childbirth
Breast Swelling vs. Postpartum Edema: What’s the Difference?
Swelling after birth can come from milk changes in your breasts or fluid shifts in the rest of your body. They feel different and improve in different ways.
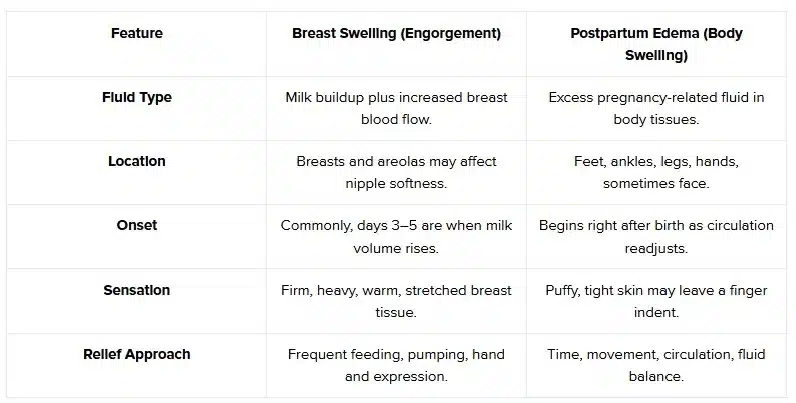

Both are common, but they come from different causes. The right relief depends on where the swelling is and what your body is adjusting to.
If you want to understand another common part of healing after birth, read next: Postpartum Bleeding: What’s Normal and When to Seek Help
When Is Postpartum Swelling NOT Normal?

Most postpartum swelling is harmless and fades as your body rebalances fluids. Certain patterns and symptoms, though, point to complications that need prompt medical care.
Here are specific warning signs that swelling may be medically urgent:
- One-Sided Leg Swelling: Sudden swelling in only one calf or thigh, especially with warmth or tenderness, can signal deep vein thrombosis requiring immediate evaluation.
- Severe Headache With Swelling: Persistent headache with facial or hand swelling and visual changes may indicate postpartum preeclampsia linked to dangerous blood pressure elevation.
- Breathlessness With Puffiness: Shortness of breath, chest pressure, or quick heartbeat alongside swelling can suggest fluid in the lungs or a pulmonary embolism.
- Fever With Localized Redness: Swelling that is hot, red, and painful in the breast, incision, or perineal area may point to infection rather than simple fluid retention.
- Persistent Pitting Edema: Skin that keeps a deep indentation after pressing, especially with quick weight gain, may reflect abnormal fluid overload or cardiovascular strain.
Trust your instincts. If swelling feels different, worsens suddenly, or comes with these symptoms, contact your provider right away.
Supporting Your Recovery While You Care for Baby
Healing after birth happens alongside round-the-clock newborn care. Small, intentional habits support tissue repair, hormone balance, and energy so you can care for your baby without draining yourself, especially if you are dealing with postpartum edema, swollen feet postpartum, or swelling ankles after a C-section.
Key recovery priorities that protect your body while you parent:
- Uterine Healing Support: Breastfeeding releases oxytocin, which causes the uterus to contract. These contractions help reduce bleeding and support the uterus, gradually returning toward its pre-pregnancy size.
- Pelvic Tissue Protection: Avoid heavy lifting and high-impact movement early on, since pelvic floor muscles and connective tissue are still stretched and regaining tensile strength.
- Incision or Perineal Care: Use warm water cleansing after bathroom visits and keep the area dry to reduce bacterial growth and support healthy wound healing.
- Iron and Blood Replenishment: If blood loss was significant, iron-rich foods or supplements help restore hemoglobin levels, improving oxygen delivery to healing tissues.
- Milk Supply Regulation: Regular milk removal, either by baby or breast pump, prevents engorgement pressure and supports stable prolactin signaling for consistent milk production.
- Lactation Guidance Access: A lactation consultant can assess latch, flange fit, and feeding patterns, helping prevent nipple trauma and providing effective milk transfer during recovery.
Your recovery is not separate from caring for your baby. When you support your healing, you build the strength and energy needed for both of you.
Final thoughts
As the body works through swelling and fluid shifts, breast fullness can add another layer of pressure and discomfort. When milk comes in, breasts may feel heavy, tight, or tender, which can make recovery feel even more overwhelming. Gentle milk removal, whether by baby or pump, can ease that pressure and help the body settle more comfortably.
Many health plans cover a breast pump under the Affordable Care Act, often with little or no out-of-pocket cost. Getting support with eligibility checks, prescription management, and insurance navigation can take one more stressor off during a time when rest and healing matter most.
FAQs
1. Why are my feet swollen after a C-section more than after a vaginal birth?
Swollen feet after a C-section are often linked to the larger amount of IV fluids given during surgery. These fluids move into tissues afterward, especially in the feet, due to gravity.
2. Is pedal edema postpartum different from regular postpartum swelling?
Pedal edema postpartum is simply swelling limited to the feet. It is a form of postpartum edema, but localized to the lower extremities rather than affecting hands, face, or legs.
3. How long does swelling ankles after a C-section usually last?
Swelling ankles after a C-section can last up to two to three weeks. Surgical fluids, limited mobility, and inflammation around the incision can slow how quickly fluid leaves the tissues.
4. Can Pitocin cause postpartum swelling after delivery?
Yes, postpartum swelling after Pitocin can happen. Pitocin affects hormone levels and fluid balance, and when combined with IV fluids, it may temporarily increase overall fluid retention.
5. When should swollen legs and feet after a C-section be checked by a doctor?
If swollen legs and feet after a C-section are uneven, painful, warm, or red on one side, it could signal a blood clot and needs urgent medical evaluation.










